WRONG ADVICE FOR CANADIANS
according to the scientists.
ALBERTA - 31 May 2019
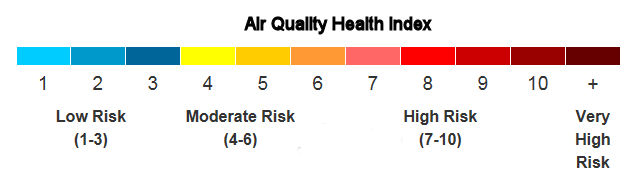
Air quality conditions in Calgary and other parts of southern Alberta were much worse on Friday. Calgarys AQHI level was a 10+ on Friday morning. That risk was forecast to remain very high into Friday night.
The Calgary Board of Education said principals make decisions based on local conditions, but the boards guidelines are to consider indoor recess and lunch for students when the AQHI reaches 10+.When it comes to other outdoor activities, Calgary Minor Soccer advises games and practices should be delayed or rescheduled if the AQHI reaches 7 or higher.
https://globalnews.ca/news/5339226/alberta-air-quality-forecast-may-31/
Look at the Index numbers below. So authorities wait for the index to get to the higher end before they protect their children from the toxic particulates. Authorities are failing in their duty of care if we read the World Health Organisations Group 1 carcinogenic substances list, ie Particulate Matter.
ALBERTA WILDFIRE ON RADIO 770CHQR
Listen to Dr. Ted Jablonski -
https://omny.fm/shows/the-morning-news-with-gord-gillies/do-masks-work-for-smoke/embed
No, smoke is primarily made up of fine particulates (PM2.5s). It does not only cause irritation and inflammation it is toxic and can also cross over into the blood stream and cause cancer in other organs.
The AQHI was at 10 and I could not believe Dr Jablonski said healthy kids could go outside in the smoke, after he had said that level equated to smoking a packet of cigarettes.
But then that doesnt surprise me when he said he goes against all the scientific health advice and goes running in Class 1 carcinogen conditions!
Canadian Air Quality Health Index is wrong and doctors should not be saying it is ok for kids with healthy lungs to be going outside in 10+ smoke in Alberta.
ALBERTA - 31 May 2019
Air quality conditions in Calgary and other parts of southern Alberta were much worse on Friday. Calgarys AQHI level was a 10+ on Friday morning. That risk was forecast to remain very high into Friday night.
The Calgary Board of Education said principals make decisions based on local conditions, but the boards guidelines are to consider indoor recess and lunch for students when the AQHI reaches 10+.When it comes to other outdoor activities, Calgary Minor Soccer advises games and practices should be delayed or rescheduled if the AQHI reaches 7 or higher.
https://globalnews.ca/news/5339226/alberta-air-quality-forecast-may-31/
Look at the Index numbers below. So authorities wait for the index to get to the higher end before they protect their children from the toxic particulates. Authorities are failing in their duty of care if we read the World Health Organisations Group 1 carcinogenic substances list, ie Particulate Matter.
ALBERTA WILDFIRE ON RADIO 770CHQR
Listen to Dr. Ted Jablonski -
https://omny.fm/shows/the-morning-news-with-gord-gillies/do-masks-work-for-smoke/embed
No, smoke is primarily made up of fine particulates (PM2.5s). It does not only cause irritation and inflammation it is toxic and can also cross over into the blood stream and cause cancer in other organs.
The AQHI was at 10 and I could not believe Dr Jablonski said healthy kids could go outside in the smoke, after he had said that level equated to smoking a packet of cigarettes.
But then that doesnt surprise me when he said he goes against all the scientific health advice and goes running in Class 1 carcinogen conditions!
Canadian Air Quality Health Index is wrong and doctors should not be saying it is ok for kids with healthy lungs to be going outside in 10+ smoke in Alberta.
From this:
17/11/2008: On the new website there is not even an air quality program.
To this:
19/7/2009 UPDATE: - Environmental smoke does not get a mention any longer.
And to this:
23/2/2012: A new DHHS-PEH website is launched called 'Wood smoke, air quality, your health.'
Public and Environmental Health believe (like Forestry) that if they advise people on the internet then they have met their responsibilities.
No they have not. They cannot make the general population responsible for something like toxic air that is harmful and out of the public's control.
DHHS is responsible for our environmental health. They cannot just palm this off onto the population by saying when your home is letting in smoky air from the outside, take a break by going to a friends place, the local library, shopping centre, or sports centre!
In the past air pollution was considered an outdoor problem.
Our P&HS fails to recognise the following:
"Potentially, indoor air pollutants can greatly exceed outdoor levels. It is important that people with asthma consider this when they seek to use their homes or other buildings as refuges from the effects of outdoor pollution." http://www.nationalasthma.org.au/health-professionals/information-papers/asthma-air-pollution-asthma-series-paper-4-/indoor-air-pollutants
Forestry comes before Health in Tasmania!
"Surely no child should have to breathe air that could kill them".
17/11/2008: On the new website there is not even an air quality program.
To this:
19/7/2009 UPDATE: - Environmental smoke does not get a mention any longer.
And to this:
23/2/2012: A new DHHS-PEH website is launched called 'Wood smoke, air quality, your health.'
Public and Environmental Health believe (like Forestry) that if they advise people on the internet then they have met their responsibilities.
No they have not. They cannot make the general population responsible for something like toxic air that is harmful and out of the public's control.
DHHS is responsible for our environmental health. They cannot just palm this off onto the population by saying when your home is letting in smoky air from the outside, take a break by going to a friends place, the local library, shopping centre, or sports centre!
In the past air pollution was considered an outdoor problem.
Our P&HS fails to recognise the following:
"Potentially, indoor air pollutants can greatly exceed outdoor levels. It is important that people with asthma consider this when they seek to use their homes or other buildings as refuges from the effects of outdoor pollution." http://www.nationalasthma.org.au/health-professionals/information-papers/asthma-air-pollution-asthma-series-paper-4-/indoor-air-pollutants
Forestry comes before Health in Tasmania!
"Surely no child should have to breathe air that could kill them".
This is what the updated version said following discussions with PEHS in July 2008.
"Action should be taken by others where possible to minimise exposure of the public to smoke. "
"Action should be taken by others where possible to minimise exposure of the public to smoke. "
According to the World Health Organisation (WHO) there is no safe level of fine particle pollution.
If your doctor asks you, "have you ever smoked?", answer "yes".
You have smoked forestry smoke.
Cigarettes smoke is burning vegetation. Forestry smoke is burning vegetation
You have smoked forestry smoke.
Cigarettes smoke is burning vegetation. Forestry smoke is burning vegetation
22.4.2010 - Dr Roscoe Taylor, Tasmanian Director of Public Health issues smoke warning.
Governments Role in Protecting Health and Safety - and again; the New England Journal of Medicine
Governments Role in Protecting Health and Safety - and again; the New England Journal of Medicine
"Our role is to monitor the health of the Tasmanian population, and put in place programs to protect or promote health."
"We do not have any regulatory role in relation to environmental smoke."
Public and Environmental Health is another agency that does not have any regulatory control over environmental smoke from planned burns.
Government's Role in Protecting Health and Safety
"Government has a responsibility to implement effective public health measures that increase the information available to the public and decision makers, protect people from harm, promote health, and create environments that support healthy behaviors. The health, financial, and productivity gains from public health actions benefit individuals and society as a whole." - Dr. Frieden, Director of the Centers for Disease Control and Prevention, Atlanta. New England Journal of Medicine
"We do not have any regulatory role in relation to environmental smoke."
Public and Environmental Health is another agency that does not have any regulatory control over environmental smoke from planned burns.
Government's Role in Protecting Health and Safety
"Government has a responsibility to implement effective public health measures that increase the information available to the public and decision makers, protect people from harm, promote health, and create environments that support healthy behaviors. The health, financial, and productivity gains from public health actions benefit individuals and society as a whole." - Dr. Frieden, Director of the Centers for Disease Control and Prevention, Atlanta. New England Journal of Medicine
DHHS - Organisational chart - July 2012; see where PEH fits in.

In 2008 this was the Tasmania Health Department's Answer to our deliberate forestry smoke problem.
No wonder the following document was never headed or signed.
What P&EH don't tell you is, that unless the building is fitted with ABSOLUTE FILTERS (SUPER HEPA FILTERS) you are breathing the same smoky air as outside, and possibly 3-5 times worse anyway. Buildings are rarely fitted with absolutes, and they are almost never fitted to homes.
I remember being inside at Belconnen Westfield to try and get a bit of a reprieve from the air, she says. And the smoke alarm started going off [inside this] massive shopping centre.
I came home to see the same thing, smoke alarms just going off and people had to come outside and stand in the smoke where they were coughing 10 times worse.
First published at https://www.theguardian.com/environment/ng-interactive/2020/feb/20/the-toxic-air-we-breathe-the-health-crisis-from-australias-bushfires
No wonder the following document was never headed or signed.
What P&EH don't tell you is, that unless the building is fitted with ABSOLUTE FILTERS (SUPER HEPA FILTERS) you are breathing the same smoky air as outside, and possibly 3-5 times worse anyway. Buildings are rarely fitted with absolutes, and they are almost never fitted to homes.
I remember being inside at Belconnen Westfield to try and get a bit of a reprieve from the air, she says. And the smoke alarm started going off [inside this] massive shopping centre.
I came home to see the same thing, smoke alarms just going off and people had to come outside and stand in the smoke where they were coughing 10 times worse.
First published at https://www.theguardian.com/environment/ng-interactive/2020/feb/20/the-toxic-air-we-breathe-the-health-crisis-from-australias-bushfires
Burning is an option, breathing is not.

Public and Environmental Health Service
Dept. of Health & Human Services (DHHS)
Dept. of Health & Human Services (DHHS)


13.2.2014 - Right to Information Decision:
Go here to find the number of air pollution, and particulate matter, susceptible people in Tasmania.
Also, being told to remain indoors only gives short-time protection from smoke. Maybe not even that depending on the building construction.
More than 3,000 Australians die every year from air-pollution-related illness; nearly twice the national road toll. - 10.Nov.2014 report by Places You Love alliance.
The US EPA has calculated that the ratio of healthcare cost savings to the costs of compliance with the Clean Air Act was 25:1 in 2010. This means that for every dollar spent complying with the Clean Air Act, twenty-five dollars were saved in healthcare costs due to lower disease burden, including a reduction in premature deaths, and reduction is cases of bronchitis, asthma, and myocardial infarction. - US Environmental Protection Agency Office of Air and Radiation. The Benefits and Costs of the Clean Air Act: 1990-2020. Washington DC: EPA, 2010
Go here to find the number of air pollution, and particulate matter, susceptible people in Tasmania.
Also, being told to remain indoors only gives short-time protection from smoke. Maybe not even that depending on the building construction.
More than 3,000 Australians die every year from air-pollution-related illness; nearly twice the national road toll. - 10.Nov.2014 report by Places You Love alliance.
The US EPA has calculated that the ratio of healthcare cost savings to the costs of compliance with the Clean Air Act was 25:1 in 2010. This means that for every dollar spent complying with the Clean Air Act, twenty-five dollars were saved in healthcare costs due to lower disease burden, including a reduction in premature deaths, and reduction is cases of bronchitis, asthma, and myocardial infarction. - US Environmental Protection Agency Office of Air and Radiation. The Benefits and Costs of the Clean Air Act: 1990-2020. Washington DC: EPA, 2010
Now known as DHHS Public Health Services
Changed from Public and Environmental Health
Changed from Public and Environmental Health
Health and sense-t
Click on the above picture to read about research happening in Tasmania.
Cleanairtas feels any research must firstly aim to reduce deliberate air pollution at the source.
Research must not be used to have susceptible groups locked away, put into masks, or put on more medication whilst harmful emissions continue.
Cleanairtas maintains it is not up to the population to have to dodge or suffer pernicious pollution caused by others, as has been suggested on this Health page and by Asthma Foundation Tasmania
When it comes to deliberate wood smoke we need to target the pollution, not try to devise individual/personal health plans and put people on medicines.....so the pollution can continue.
I hope this is where we are headed?
Click on the above picture to read about research happening in Tasmania.
Cleanairtas feels any research must firstly aim to reduce deliberate air pollution at the source.
Research must not be used to have susceptible groups locked away, put into masks, or put on more medication whilst harmful emissions continue.
Cleanairtas maintains it is not up to the population to have to dodge or suffer pernicious pollution caused by others, as has been suggested on this Health page and by Asthma Foundation Tasmania
When it comes to deliberate wood smoke we need to target the pollution, not try to devise individual/personal health plans and put people on medicines.....so the pollution can continue.
I hope this is where we are headed?
Asthma sufferers to get air alert - smartphone app launched October 28, 2015
Clean air: the health and economic arguments
Asthma costs Australia almost $28b every year - 24/11/2015
Asthma costs Australia almost $28b every year - 24/11/2015
Fire, smoke, climate change. Listen to Dr Fay Johnston on ABC Radio National - 6/2/2016
Most jurisdictions throughout Australia have approved (in legislation/regulation) prescribed burning however they have failed to consider /ignored the serious health effects that these fires have on local communities
Pioneering Personalised Allergy Medicine:
Climate change is having a significant impact on the health of people susceptible to pollen allergies. Higher air temperatures and rising carbon dioxide levels are stimulating plant growth, increasing the production of airborne allergens and extending the seasons during which symptoms are most common. However, maintaining a personalised record of pollen sensitivity is an effective method of limiting exposure to the triggers and treating the debilitating effects, particularly in children.
Climate change is having a significant impact on the health of people susceptible to pollen allergies. Higher air temperatures and rising carbon dioxide levels are stimulating plant growth, increasing the production of airborne allergens and extending the seasons during which symptoms are most common. However, maintaining a personalised record of pollen sensitivity is an effective method of limiting exposure to the triggers and treating the debilitating effects, particularly in children.
Interesting health research is being conducted in Tasmania.
It is highly recommended to watch Prof. Graeme Zosky's seminar "Air pollution and health: How particulate matter leads to illness", and
Dr Fay Johnson's seminar "The AirRater App: How citizen science can reduce health impacts from atmospheric hazards"
These and other Centre for Air pollution, energy and health research (CAR) seminars can be found HERE
It is highly recommended to watch Prof. Graeme Zosky's seminar "Air pollution and health: How particulate matter leads to illness", and
Dr Fay Johnson's seminar "The AirRater App: How citizen science can reduce health impacts from atmospheric hazards"
These and other Centre for Air pollution, energy and health research (CAR) seminars can be found HERE
Wildland fire smoke research to study impact on children's immune system
Dr. Prunicki and her team at the Stanford School of Medicine believe wildland fire smoke is more toxic than smoke from forest fires because of the plastics and metal burned during a major conflagration.
Dr. Prunicki and her team at the Stanford School of Medicine believe wildland fire smoke is more toxic than smoke from forest fires because of the plastics and metal burned during a major conflagration.
Air pollution linked to thickness of arteries
Researchers studied the impact of particulate matter such as that found in smoke and haze and having a diameter of less than 2.5 microns on the health of individuals. They specifically looked at the carotid intima-media thickness (CIMT) or the thickness of key arteries, a marker of cardiovascular risk.
Researchers studied the impact of particulate matter such as that found in smoke and haze and having a diameter of less than 2.5 microns on the health of individuals. They specifically looked at the carotid intima-media thickness (CIMT) or the thickness of key arteries, a marker of cardiovascular risk.
With Californias wildfire season bringing yearly evacuations, damage to communities and lasting health effects, Stanford faculty have been exploring ways of preventing fires and managing health risks.
A mother's exposure to particulate air pollution during pregnancy is associated with reduced cardiac response to stress in six-month-old infants.
This study is the first to find that particulate air pollution exposure in utero can affect heart rate variability, which is a known risk factor for health issues
This study is the first to find that particulate air pollution exposure in utero can affect heart rate variability, which is a known risk factor for health issues
Air pollution tied to hospitalizations for a wide range of illnesses
Short-term exposure to fine particulate matter was associated with an increased risk of several common causes of hospital admissions including sepsis or septicemia, a life-threatening reaction to a bacterial infection in the bloodstream; fluid and electrolyte disorders; kidney failure; and intestinal obstructions. These diseases have rarely been studied in the context of PM 2.5 and hospitalizations, the study team writes
Short-term exposure to fine particulate matter was associated with an increased risk of several common causes of hospital admissions including sepsis or septicemia, a life-threatening reaction to a bacterial infection in the bloodstream; fluid and electrolyte disorders; kidney failure; and intestinal obstructions. These diseases have rarely been studied in the context of PM 2.5 and hospitalizations, the study team writes
Leaders ignore NSW 5 fires and smoke at the cost of worsening mental health
"Clearly we do not have a national consensus. What we have is division, we have arguments and we have screaming matches (in Parliament). The place is burning down. If we are not discussing it today, if not, when?" - Prof. Ian Hickie
"Clearly we do not have a national consensus. What we have is division, we have arguments and we have screaming matches (in Parliament). The place is burning down. If we are not discussing it today, if not, when?" - Prof. Ian Hickie
Dirty Air and the Human Brain: Does Pollution Poison the Mind?
In recent years, new areas of study have opened up into how air pollution might affect our minds and the way we think and feel. Epidemiologists and neuroscientists have found evidence linking long-term exposure to air pollution with increased incidence of dementia, Alzheimers Disease and other brain maladies. At the same time, behavioral and labor economists have published a series of papers about the effects of air pollution on cognitive performance.
In recent years, new areas of study have opened up into how air pollution might affect our minds and the way we think and feel. Epidemiologists and neuroscientists have found evidence linking long-term exposure to air pollution with increased incidence of dementia, Alzheimers Disease and other brain maladies. At the same time, behavioral and labor economists have published a series of papers about the effects of air pollution on cognitive performance.
According to Brazils INPE (National Institute for Space Research), the country faced a recorded 72,843 fire outbreaks from Jan 1 to Aug 19, 2019.
The number was 83% higher than during the same period last year, when 39, 759 fire outbreaks were recorded.
The number was 83% higher than during the same period last year, when 39, 759 fire outbreaks were recorded.
Eco-anxiety - what it is and how to manage it.
According to a 2018 national survey almost 70% of people in the United States are worried about climate change, and around 51% feel "helpless."
According to a 2018 national survey almost 70% of people in the United States are worried about climate change, and around 51% feel "helpless."
Air pollution Vs number of cigarettes smoked.
Here is the rule of thumb: one cigarette per day is the rough equivalent of a PM2.5 level of 22 µg/m3. Double that level, and it is equivalent to 2 cigarettes per day. Of course, unlike cigarette smoking, the pollution reaches every age group.
Here is the rule of thumb: one cigarette per day is the rough equivalent of a PM2.5 level of 22 µg/m3. Double that level, and it is equivalent to 2 cigarettes per day. Of course, unlike cigarette smoking, the pollution reaches every age group.
Potential health effects from exposure to particulate matter:
Short-term and long-term exposure is thought to have different mechanisms of effect. Short-term exposure appears to exacerbate pre-existing diseases while long-term exposure most likely causes disease and increases the rate of progression.
Short-term exposure (hours to days) can lead to:
Irritated eyes, nose and throat
Worsening asthma and lung diseases such as chronic bronchitis (also called chronic obstructive pulmonary disease or COPD)
Heart attacks and arrhythmias (irregular heart beat) in people with heart disease
Increases in hospital admissions and premature death due to diseases of the respiratory and cardiovascular systems
Long-term exposure (many years) can lead to:
Reduced lung function
Development of cardiovascular and respiratory diseases
Increased rate of disease progression
Reduction in life expectancy
Short-term and long-term exposure is thought to have different mechanisms of effect. Short-term exposure appears to exacerbate pre-existing diseases while long-term exposure most likely causes disease and increases the rate of progression.
Short-term exposure (hours to days) can lead to:
Irritated eyes, nose and throat
Worsening asthma and lung diseases such as chronic bronchitis (also called chronic obstructive pulmonary disease or COPD)
Heart attacks and arrhythmias (irregular heart beat) in people with heart disease
Increases in hospital admissions and premature death due to diseases of the respiratory and cardiovascular systems
Long-term exposure (many years) can lead to:
Reduced lung function
Development of cardiovascular and respiratory diseases
Increased rate of disease progression
Reduction in life expectancy
Study lead author Kazuaki Negishi, from the University of Sydney School of Medicine, said despite recent concerns about rising PM2.5 levels, residents are "blindly" assuming air quality is safe at levels below 25 µg/m3, when there is really "no safe level" of PM2.5 pollution. Professor Negishi said the DPIE index indicating air quality may be "fair", "good" or "very good" at thresholds above zero and below 25 µg/m3 "might give us false reassurance" and let polluters off the hook.
Originally sighted as:" Short-term exposure to ambient fine particulate matter and out-of-hospital cardiac arrest: a nationwide case-crossover study in Japan
Originally sighted as:" Short-term exposure to ambient fine particulate matter and out-of-hospital cardiac arrest: a nationwide case-crossover study in Japan
Hundreds turn up to hospitals, walk-in centres during peak of smoke haze
Pollution levels peaked on New Year's Day when some parts of Canberra recorded daily average PM2.5-particle levels of almost 5000.
Anything above 200 is considered hazardous
Pollution levels peaked on New Year's Day when some parts of Canberra recorded daily average PM2.5-particle levels of almost 5000.
Anything above 200 is considered hazardous
Bushfire royal commission hears that Black Summer smoke killed nearly 450 people.
Associate Professor Fay Johnston, from the Menzies Institute for Medical Research at the University of Tasmania, said her team estimated around 445 people died as a result of the smoke, over 3,000 people were admitted to hospital for respiratory problems and 1,700 people presented for asthma.
Associate Professor Fay Johnston, from the Menzies Institute for Medical Research at the University of Tasmania, said her team estimated around 445 people died as a result of the smoke, over 3,000 people were admitted to hospital for respiratory problems and 1,700 people presented for asthma.
Logging increases bush flammability for 30 years, research shows.
The meta-study which assessed 51 peer-reviewed papers found logging increased the severity of forest fires from about 10 years after the trees are extracted with effects lasting more than three decades.
The meta-study which assessed 51 peer-reviewed papers found logging increased the severity of forest fires from about 10 years after the trees are extracted with effects lasting more than three decades.
Long-term exposure to air pollution appears to have a significant influence on outcomes for people hospitalised with Covid-19, according to a large observational study conducted by the European Society of Clinical Microbiology and Infectious Diseases
BREATHE, a Kirby Institute research study in 2021
Bushfire smoke, asthma, lung disease and masks
The aim of this research is to determine whether the use of surgical masks and P2 masks protects people with asthma, emphysema, chronic bronchitis or bronchiectasis from the effects of smoke exposure during bushfire season in Australia. We will compare exposure reduction methods, including surgical masks, P2 mask facemasks, and avoiding outdoor activities. There is no clinical efficacy data to support the choice and use of facemasks, P2 masks or staying indoors for protection against bushfire smoke.
However, lung diseased candidates should not be signed up for Health Ethics reasons to wear surgical masks which do not stop wood smoke.
Bushfire smoke, asthma, lung disease and masks
The aim of this research is to determine whether the use of surgical masks and P2 masks protects people with asthma, emphysema, chronic bronchitis or bronchiectasis from the effects of smoke exposure during bushfire season in Australia. We will compare exposure reduction methods, including surgical masks, P2 mask facemasks, and avoiding outdoor activities. There is no clinical efficacy data to support the choice and use of facemasks, P2 masks or staying indoors for protection against bushfire smoke.
However, lung diseased candidates should not be signed up for Health Ethics reasons to wear surgical masks which do not stop wood smoke.

Travelling lung exhibit makes stop in Calgary, shows how pollution affects air we breathe - click on photo for story
A traveling exhibit is aiming to drive conversation about air pollution.
Lungs in the Air, featuring a pair of 10-metre inflatable lungs, made a stop in Calgarys East Village Saturday, coinciding with World Lung Day on 25th September 2021
A traveling exhibit is aiming to drive conversation about air pollution.
Lungs in the Air, featuring a pair of 10-metre inflatable lungs, made a stop in Calgarys East Village Saturday, coinciding with World Lung Day on 25th September 2021
Studies show that climate change has had a large impact on mental health within the last few years. Young people especially are suffering. It was reported that 45% of young adults and teenagers feel that climate anxiety affects their daily life.
Its crucial to remember that climate anxiety should not be dismissed as overreacting - it's a healthy response to an existential threat. Thats why my team at EcoWatch created a resource highlighting ways to manage this anxiety
Its crucial to remember that climate anxiety should not be dismissed as overreacting - it's a healthy response to an existential threat. Thats why my team at EcoWatch created a resource highlighting ways to manage this anxiety
Exposure to Air Pollution Could Trigger Heart Attack Within an Hour, Study Finds
Even low levels of exposure to air pollutants could trigger a heart attack within an hour, according to a recent study in China.1
The study, published in the journal Circulation, evaluated more than 1 million cases of acute coronary syndrome (ACS) over the course of five years. Researchers measured the impact of four common pollutants: fine particulate matter (PM2.5 and PM10), nitrogen dioxide, sulfur dioxide, and carbon monoxide. The results suggested that short-term exposure to any level of these pollutants was associated with the onset of ACS.
Even low levels of exposure to air pollutants could trigger a heart attack within an hour, according to a recent study in China.1
The study, published in the journal Circulation, evaluated more than 1 million cases of acute coronary syndrome (ACS) over the course of five years. Researchers measured the impact of four common pollutants: fine particulate matter (PM2.5 and PM10), nitrogen dioxide, sulfur dioxide, and carbon monoxide. The results suggested that short-term exposure to any level of these pollutants was associated with the onset of ACS.
Air pollution exposure may hasten death, even at levels deemed 'safe,' study says
The nationwide study of more than 60 million senior citizens linked long-term exposure to two main smog pollutants ozone and fine particulate matter to an increased risk of premature death.
The analysis found no sign of a safe level of pollution, below which the risk of dying early tapered off.
The nationwide study of more than 60 million senior citizens linked long-term exposure to two main smog pollutants ozone and fine particulate matter to an increased risk of premature death.
The analysis found no sign of a safe level of pollution, below which the risk of dying early tapered off.

AIR POLLUTION
Written by Pete Knapp, air quality researcher at Imperial College London
Do you know anyone who has an allergy or asthma? Or anyone who had a stroke, suffering dementia, or died from heart disease?
Air pollution is likely to have been a contributor.
Written by Pete Knapp, air quality researcher at Imperial College London
Do you know anyone who has an allergy or asthma? Or anyone who had a stroke, suffering dementia, or died from heart disease?
Air pollution is likely to have been a contributor.
New study shows the health impacts of biomass smoke exposure in Tasmania
Results from this study were published in the International Journal of Environmental Research and Public Health and found that over 10 years, biomass smoke was linked to an estimated 69 deaths, 86 hospital admissions, and 15 asthma Emergency Department visits in Tasmania each year, with over 74% of these cases attributed to wood heater smoke. The study estimated that in Tasmania the average yearly health costs were AUD $293 million for wood heater smoke. This translates into health costs equivalent to AUD $4232 per wood heater each year across the state.
Results from this study were published in the International Journal of Environmental Research and Public Health and found that over 10 years, biomass smoke was linked to an estimated 69 deaths, 86 hospital admissions, and 15 asthma Emergency Department visits in Tasmania each year, with over 74% of these cases attributed to wood heater smoke. The study estimated that in Tasmania the average yearly health costs were AUD $293 million for wood heater smoke. This translates into health costs equivalent to AUD $4232 per wood heater each year across the state.
Health-care waste WHO
Of the total amount of waste generated by health-care activities, about 85% is general, non-hazardous waste.
The remaining 15% is considered hazardous material that may be infectious, toxic or radioactive.
Every year an estimated 16 billion injections are administered worldwide, but not all of the needles and syringes are properly disposed of afterwards.
Open burning and incineration of health care wastes can, under some circumstances, result in the emission of dioxins, furans, and particulate matter.
Measures to ensure the safe and environmentally sound management of health care wastes can prevent adverse health and environmental impacts from such waste including the unintended release of chemical or biological hazards, including drug-resistant microorganisms, into the environment thus protecting the health of patients, health workers, and the general public.
Of the total amount of waste generated by health-care activities, about 85% is general, non-hazardous waste.
The remaining 15% is considered hazardous material that may be infectious, toxic or radioactive.
Every year an estimated 16 billion injections are administered worldwide, but not all of the needles and syringes are properly disposed of afterwards.
Open burning and incineration of health care wastes can, under some circumstances, result in the emission of dioxins, furans, and particulate matter.
Measures to ensure the safe and environmentally sound management of health care wastes can prevent adverse health and environmental impacts from such waste including the unintended release of chemical or biological hazards, including drug-resistant microorganisms, into the environment thus protecting the health of patients, health workers, and the general public.
Effect of short-term exposure to ambient nitrogen dioxide and particulate matter on repeated lung function measures in infancy
The developing lung is highly susceptible to environmental toxicants, with both short- and long-term exposure to ambient air pollutants linked to early childhood effects. This study assessed the short-term exposure effects of nitrogen dioxide (NO2) and particulate matter (PM10) on lung function in infants aged 6 weeks, 6, 12 and 24 months, the early developmental phase of child growth.
The developing lung is highly susceptible to environmental toxicants, with both short- and long-term exposure to ambient air pollutants linked to early childhood effects. This study assessed the short-term exposure effects of nitrogen dioxide (NO2) and particulate matter (PM10) on lung function in infants aged 6 weeks, 6, 12 and 24 months, the early developmental phase of child growth.
Researchers suggest air pollution be included as risk factor for lung cancer in non-smokers
To assess the connection between pollution and lung cancer diagnosis, Dr Renelle Myers compared the cumulative three-year versus 20-year exposure in females with newly diagnosed lung cancer who have never smoked.
To assess the connection between pollution and lung cancer diagnosis, Dr Renelle Myers compared the cumulative three-year versus 20-year exposure in females with newly diagnosed lung cancer who have never smoked.
High Air Pollution Level is Creating Physical and Mental Health
December 4, 2022 Exposure to high level of air pollution significantly raises the risks of breathing difficulties, cough, lower respiratory tract infections, as well as depression and other health conditions. Children under five years, elderly, and people with comorbidities such as diabetes, heart or respiratory conditions, are most vulnerable, says a new World Bank report launched today.
December 4, 2022 Exposure to high level of air pollution significantly raises the risks of breathing difficulties, cough, lower respiratory tract infections, as well as depression and other health conditions. Children under five years, elderly, and people with comorbidities such as diabetes, heart or respiratory conditions, are most vulnerable, says a new World Bank report launched today.
ETHICAL OR NOT?
SURGICAL MASKS PROVIDE LITTLE OR NO PROTECTION FROM WOOD SMOKE, NO MATTER WHAT THE SOURCE.
GROUP (1) Participants will be required to wear a SURGICAL MASK when the Air Quality Index (AQI) is poor or there is a fire alert.
On the 2nd August 20223 cleanairtas emailed the contact Dr Elizabeth Kpozehouen - Research Associate, Biosecurity Program, indicating a desire to register as an interested person, not as a participant.
On the 8th of October 2023 cleanairtas emailed NSW Human Ethics and Chief Investigator and Prof. Raina MacIntyre - Professor and Head of Biosecurity Research Program with concerns part of this study was unethical.
Note: Further information can be found down the bottom at https://cleanairtas.com/correspondence/correspondence.html
Baggy blue surgical masks were not designed to filter incoming air. They were designed to stop outgoing spit from the wearer.
The filtration factor of baggy blue surgical masks is about 30%.
This means the wearer is breathing about 70% unfiltered air, more if it has big gaps up the sides.
And yet in this BREATHE Study, asthma/COPD etc. participants were required to wear a surgical mask during high episodes of smoke.
How ethical is that?
SURGICAL MASKS PROVIDE LITTLE OR NO PROTECTION FROM WOOD SMOKE, NO MATTER WHAT THE SOURCE.
GROUP (1) Participants will be required to wear a SURGICAL MASK when the Air Quality Index (AQI) is poor or there is a fire alert.
On the 2nd August 20223 cleanairtas emailed the contact Dr Elizabeth Kpozehouen - Research Associate, Biosecurity Program, indicating a desire to register as an interested person, not as a participant.
On the 8th of October 2023 cleanairtas emailed NSW Human Ethics and Chief Investigator and Prof. Raina MacIntyre - Professor and Head of Biosecurity Research Program with concerns part of this study was unethical.
Note: Further information can be found down the bottom at https://cleanairtas.com/correspondence/correspondence.html
Baggy blue surgical masks were not designed to filter incoming air. They were designed to stop outgoing spit from the wearer.
The filtration factor of baggy blue surgical masks is about 30%.
This means the wearer is breathing about 70% unfiltered air, more if it has big gaps up the sides.
And yet in this BREATHE Study, asthma/COPD etc. participants were required to wear a surgical mask during high episodes of smoke.
How ethical is that?

30.01.2024 - 1840hrs: I attended the Urgent Care Clinic in Launceston with breathing difficulties. I was referred to the Emergency Department at the Launceston General Hospital.
1912hrs: I arrived at the LGH ED.
31.01.2024 - 0055hrs After no treatment I discharged myself.
l applied under Right to Information to access my medical information.
I disputed the record of this event.
Here is the Tasmanian Health Service LGH response.
1912hrs: I arrived at the LGH ED.
31.01.2024 - 0055hrs After no treatment I discharged myself.
l applied under Right to Information to access my medical information.
I disputed the record of this event.
Here is the Tasmanian Health Service LGH response.